A Helping Hand

Recovering from surgery puts a physical strain on your body. It is important to keep moving to improve your recovery and get plenty of rest as well. It is likely you will be more tired than usual. This is where extra help from friends and family can be very important. It may be worth making arrangements with friends and family beforehand to help with day-to-day tasks. This might include getting help with looking after children, elderly relatives or pets, or help with shopping and cooking after you get home.
Eating and Drinking
After surgery, you should aim to eat a healthy balanced diet to provide the energy and nutrients your body needs to recover. You should also keep yourself well hydrated. You may find that your appetite is reduced. It may be easier to eat and drink small amounts more often. You may find foods affect you differently. Introducing foods gradually in small portions can help identify any which cause problems.
Bowel Habit

Constipation
It’s not uncommon to become constipated after surgery, some pain killers can make this worse. Try to:
- Drink plenty of fluids – aim for 8 – 10 cups per day
- Eat food high in fibre such as wholemeal bread and cereal, fruit, vegetables, beans and pulses.
- Mobilise early after surgery
Diarrhoea
- Drink plenty of fluids to avoid dehydration
- Reduce high fibre foods for a short period of time
- Avoid fatty or fried foods, spicy food and tea or coffee
- Eat little and often
If you continue to lose weight after your operation, please speak to your GP. They will be able to give you some advice and may refer you to a dietician.
Mobility and Exercise
It is important to keep active during your recovery – this has many benefits:

You should gradually increase the amount you are doing each day, aiming to walk a little bit further, or for a bit longer, each time.
Why not ask your family and friends to help you with this? Visits and phone calls from family and friends can cheer you up and encourage you to reach your goals.
Rest to Recover
Recovering from surgery puts an extra physical strain on the body so it is important when you are not being active that you get good amounts of rest.
Good quality sleep is also really important. Be careful that you don’t tire yourself out from too many visitors.
Pain Relief
As you recover from your operation your pain will improve and the amount of pain medicine you need will decrease.
By the time you are ready to go home, you may still be taking some painkillers. It is important that you continue to gradually reduce the amount you are taking after you go home. The doctors and nurses will help provide you with a plan for how to do this.
If you are taking strong painkillers, such as long-acting opioids, you should aim to gradually reduce and stop these within 2 weeks. You may need the occasional dose of short-acting opioid, but should not be using these for longer than 4 weeks after you go home.
If you feel like you still need strong painkillers for more than 4 weeks after going home, it is important to discuss this with your GP.
Wound Care
Before you leave hospital the nurses will show you how to look after your wound and provide you with spare bandages and dressings.
If you have stitches, or staples, that need removed you should make an appointment with the nurse at your GP surgery 10 – 14 days after your operation.
It is important that you keep your wound clean and dry to give it the best chance of healing.
You should look out for signs of a wound infection:
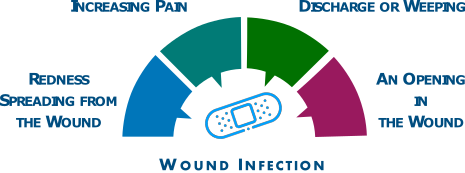
If you have any concerns about your wound, please speak to your GP or call NHS 24 on 111
Driving
If you drive, it is important that you do not return to driving before you are ready.

Strong painkillers can affect your concentration and make you more sleepy. You should not drive while you are still taking strong painkillers.
There are two important tests you should do to check that you are ready to drive:
Make an emergency stop without pain – sit in the driver’s seat and press very firmly on the brake pedal to check
Be able to turn freely to look over both shoulders – make sure you can easily see both blind spots
If you have any concerns about your ability to drive you should speak to your GP. If you are still not able to drive 3 months after your operation you should tell the DVLA.

Click here to visit the DVLA website
You could be fined up to £1,000 if you do not tell DVLA about a condition that might affect your ability to drive safely. You could also be prosecuted if you have an accident.
Time Off Work
If you work, the amount of time you need off will be different for everybody. It will depend on the:
- Type of operation you’ve had
- Type of job you do
- Speed of your recovery
Speak to the doctors looking after you in hospital before you leave about how much time you should take off.
Phased Return
Returning to normal activities, including returning to work, is an important part of your recovery.
You should speak to your employer about going back to work. It may be possible for you to have a phased return. This is where you return to work but do fewer hours, or less physical work, at the start, and then gradually increase how much you do.
Letter for your Employer
If you need less than 1 week off work you do not need a letter from a doctor and can self-certify.
If you are likely to need more than 1 week off work the doctors on the ward can give you a letter before you leave hospital. If you end up needing longer off work than originally planned, you should speak to your GP.
Getting Home
You won’t be able to drive home after your operation and will need a responsible adult to pick you up, or accompany you in a taxi.
Before you leave the hospital the nurses will go through your medication with you. They will tell you about any changes to your mediation or any new medicines. They will also make sure you have a good supply of each medicine.
When you leave hospital, a letter will be sent to your GP telling them about your operation and any changes to your medicines.
Sources of Support
Before leaving check with your nurse who to contact at the hospital if you have any problems or concerns once at home.
Additional support may be available from your GP or NHS 24 on 111















